Files
Download Full Text (435 KB)
Program
General Surgery
Training Level
Resident PGY 3
Institution
Henry Ford Macomb
Abstract
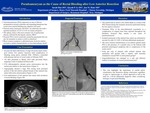
Introduction: A pseudoaneurysm (PSA) represents an area of fibrous encapsulation around a pulsatile and expanding hematoma that occurs from arterial bleeding into adjacent soft tissue1. Visceral artery aneurysms and PSAs are relatively rare with a reported incidence of 0.01 to 0.2% in routine autopsies2. The splenic artery is the most common site of aneurysmal disease, followed by the hepatic arteries, and SMA2. Visceral PSA is most commonly caused by pancreatitis but can also be traumatic in nature as well as infectious2. The most common symptom is abdominal pain; however rupture can lead to melena, hematochezia, or even hemorrhagic shock2. Case Presentation: This is the case of a 66-year-old male with history of stage 4A rectal cancer status-post robotic low anterior resection with complication of bleeding along pelvic sidewall (EBL 1500mL), controlled with pressure and use of vessel sealer in February 2018. He then presented in March 2019 with per-rectal bleed, requiring 2 units of packed red blood cells. CTA abdomen/pelvis ordered during admission showed active extravasation into the rectum just inferior to the anastomosis. Angiography was performed and showed a large PSA arising from proximal portion of the left inferior gluteal branch of the internal iliac artery with active extravasation. Coil embolization of left internal iliac artery performed with resolution of rectal bleeding. Discussion: This patient had an arterio-colic fistula likely as a result of the PSA formed during the traumatic dissection performed during his low anterior resection. Traumatic PSAs of the intra-abdominal vasculature as a complication of surgery have been reported throughout the literature; however they remain a rare cause of pseudoaneurysm4. Isolated aneurysms of the internal iliac artery are estimated to account for only 0.3–0.4% of all intra-abdominal aneurysms4. The most common manifestation of an inferior gluteal artery PSA is the presence of a painful mass in the buttock with potential neurological symptoms due to compression of the sciatic nerve3. Forty percent of patients with isolated internal iliac aneurysms will present with a rupture, with mortality estimated to exceed 50% in such patient groups4. Angioembolization has emerged as a safe and effective method of treatment of visceral pseudoaneurysms4. Conclusion: This case highlights the importance of careful pelvic visualization and dissection during colectomies regardless of open vs. laparoscopic vs. robotic approach as well as the need for a broad differential diagnosis when considering etiologies of per-rectal bleeding.
Presentation Date
5-2019
Recommended Citation
Diaz, Sarah; Lee, Quynh; and Hain, Jon, "Pseudoaneurysm as the Cause of Rectal Bleeding after Low Anterior Resection" (2019). Case Reports. 103.
https://scholarlycommons.henryford.com/merf2019caserpt/103