Files
Download Full Text (2.8 MB)
Program
WSU Medical School
Training Level
Medical Student
Institution
Wayne State University
Abstract
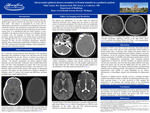
An 11-year-old African-American male presented to the emergency department with complaints of cough, fever, and runny nose for several days and headache for one day. Review of systems was positive for chills, fatigue, loss of appetite, congestion, nausea, vomiting, and facial swelling. On physical examination, the patient appeared mildly distressed and was tachycardic. Laboratory tests revealed leukocytosis with a left shift. Chest radiograph was normal. Due to the new-onset headache, nausea, vomiting and facial swelling, a non-contrast CT was obtained, which showed frontal sinusitis with concern for intracranial extension. The patient was then transferred to Children’s Hospital of Michigan where CT sinuses with contrast and MRI brain confirmed meningitis and a frontal epidural abscess. The patient was hospitalized for ten days where he underwent functional endoscopic sinus surgery and was started on four-week course of intravenous meropenem. The clinical course was complicated by a single seizure, after which levetiracetam was started. At the most recent follow-up visit nearly three months after diagnosis, the patient is doing well with no neurologic sequela.An epidural abscess (EDA) is a localized collection of pus within the epidural space, which is between the outer layer of the dura and the inner skull. The abscess is surrounded by an outer wall of inflammatory cells that have accumulated in an attempt to resolve and contain the infection. One mechanism of intracranial EDA formation is via direct spread of infection from the frontal sinus into the anterior cranial fossa. It is hypothesized that the frontal skeleton is more vulnerable to the spread of infection because of its abundant network of diploic veins, the frequency of frontal and anterior ethmoid infections, and the rapid growth of the frontal sinuses in adolescents [1]. Although EDAs are rare, occurring in less than 10% of sinus infections [2], they can have devastating consequences. Reported mortality rates for intracranial complications of sinusitis are as high as 10%–20%, and long-term neurologic morbidity, such as hemiparesis, occurs in 13%–35% of survivors [1].Symptoms of EDA occur due to slowly increasing intracranial pressure secondary to mass effect and can cause neurological deficits leading to altered mental status. If physical exam findings and patient history are suspicious for intracranial complication from sinusitis, imaging is necessary for diagnosis. In fact, the American College of Radiology appropriateness criteria recommends CT and MRI of the head and paranasal sinuses with IV contrast as complementary examinations when evaluating potential complications of sinusitis [3]. On both modalities, an epidural collection will not cross suture lines, due to the dura being tightly adhered to the inner skull at the sutures, but can cross the midline above the falx cerebri. CT findings of EDA include a low-density, lenticular-shaped, extradural fluid collection with an enhancing rim [4]. The appearance on MRI includes T2 hyperintensity with variable T1 signal (depending on the relative proteinaceous or hemorrhagic content) with surrounding rim enhancement [4].Treatment of epidural abscess typically involves a drainage procedure coupled with antibiotic therapy to eradicate the underlying infectious agent. Once treatment begins, it is often successful at both stopping the progression of the infection and reversing many of the neurological complications. As such, a timely and accurate diagnosis is imperative. In summary, intracranial epidural abscess can result in significant morbidity and mortality and should be included in the differential diagnosis for pediatric patients with acute sinusitis who present with fever, severe headache, photophobia, or other neurologic findings.
Presentation Date
5-2019
Recommended Citation
Taylor, NIkki; Saad, Hanna; and Ledbetter, Karyn, "Epidural abscess secondary to frontal sinusitis in a pediatric patient" (2019). Case Reports. 114.
https://scholarlycommons.henryford.com/merf2019caserpt/114