Files
Download Full Text (358 KB)
Program
WSU Medical School
Training Level
Medical Student
Institution
Wayne State University
Abstract
INTRODUCTION: Porokeratosis is a disorder of keratinization that comprises a heterogenous group of conditions characterized by atrophic patches bordered by a clinically and histologically distinctive hyperkeratotic ridge known as the coronoid lamella. Its most common variant, disseminated superficial actinic porokeratosis (DSAP), is most commonly inherited in an autosomal dominant manner, however, immunosuppression has been shown to induce sporadic disease. Exacerbation of preexisting DSAP lesions represents a subset of acute disseminated eruptions of porokeratosis. We report a case of bullous eruptive disseminated porokeratosis after human herpesvirus 3 (HHV-3) reactivation in an immunosuppressed patient with organ transplantation.
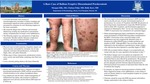
CASE REPORT: A 70-year-old female with a history of immunosuppression secondary to kidney transplant and DSAP presented to the Dermatology clinic for evaluation of a new blistering eruption on her lower extremities. The patient noted the abrupt onset of blisters and increased bilateral leg swelling one month prior to presentation during a hospitalization for herpes zoster ophthalmicus. This eruption was unresponsive to high-dose furosemide, thrombo-embolic-deterrent compression stockings, and topical clobetasol 0.05% cream. Examination revealed numerous irregularly shaped, red-brown macules surrounded by a keratotic rim of scale, clinically consistent with porokeratosis, overlying the thighs, shins, and ankles bilaterally. Within many of these characteristic porokeratosis lesions, tense vesicles and small bullae containing clear fluid were noted. Lower extremity pitting edema to the knees was appreciated as well. These findings led to a diagnosis of eruptive disseminated porokeratosis with the unusual feature of bulla formation in the setting of peripheral edema. Leg compression and elevation were advised, and the bullous porokeratosis improved at follow up.
DISCUSSION: The term eruptive disseminated porokeratosis (EDP) has been used to describe all cases of acute, disseminated eruptions of porokeratosis. In a review of 35 patients with EDP, preexisting porokeratosis (especially DSAP) had been noted in about 30% of patients, and dissemination appeared to represent an inflammatory flare. While immunosuppression likely contributed to this patient’s initial development of DSAP following kidney transplantation, the HHV-3 reactivation of her concurrent herpes zoster ophthalmicus may have triggered the abnormal clones of keratinocytes within DSAP lesions to further proliferate and manifest as EDP. Although HHV-3 has never been directly implicated in the development of EDP, herpes simplex virus infection has been reported as a possible trigger. EDP with secondary bullous changes is an exceptionally rare variant with only two cases reported in the literature to date. The bullous changes seen in our patient are suspected to be secondary to underlying edema. Abnormal keratinocytes affected by porokeratosis fail to provide adequate junctions and allow localized extravasation of interstitial fluid within the sites of reduced skin integrity. In summary, we report an unusual presentation of bullous EDP likely triggered by herpes zoster ophthalmicus in the setting of acute-on-chronic edema in a renal transplant recipient on systemic immunosuppression. Clinicians should be aware that EDP may present with bullous changes, particularly in the setting of edema.
Presentation Date
5-2019
Recommended Citation
Ellis, Morgan; Fidai, Chelsea; and Kerr, Holly, "A Rare Case of Bullous Eruptive Disseminated Porokeratosis" (2019). Case Reports. 124.
https://scholarlycommons.henryford.com/merf2019caserpt/124