Files
Download Full Text (674 KB)
Program
Neurology
Training Level
Resident PGY 2
Institution
Henry Ford Hospital
Abstract
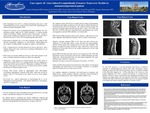
Introduction: John Cunningham virus (JCV) is a human polyomavirus that causes a fatal demyelinating disease of the central nervous system (CNS) called progressive multifocal leukoencephalopathy (PML). Primary JCV infection usually occurs asymptomatically in childhood and may result in a chronic asymptomatic carrier state. It remains usually dormant in the kidneys, lympho-reticular system, or brain tissue. Seventy to ninty percent of adults are seropositive for the JC virus and the viral DNA is detected in the urine of 20%-30% of immunologically intact adults. Reactivation of JCV is seen commonly in the setting of HIV infection, hematologic malignancy, or iatrogenic immunosuppression due to failure of cellular immune surveillance to suppress viral replication. PML lesions are typically multifocal, non-contrast enhancing at the grey white matter junction, usually in the parietooccipital, peri-thalamic regions, cerebellum, and brain stem. We present an immunocompromised patient with PML induced longitudinally extensive transverse myelitis (LETM) and peripheral nerve root involvement. Case report: 62 years old male presented with progressive weakness and difficulty walking for less than a month. The patient was diagnosed with chronic lymphocytic leukemia in 2009. He was managed with monthly intravenous immunoglobulins, as he developed hypogammaglobinemia after only two sessions of chemotherapy with Fludarabine and Rituximab. He remained asymptomatic till August 2018, when he developed left leg weakness that rapidly extended to involve the right leg in a month. Shortly thereafter, he developed urinary and fecal incontinence and became bed ridden. His examination showed bilateral lower extremity hypotonia, absent deep tendon reflexes and prominent fasciculations. Cerebrospinal fluid (CSF )analysis showed 2 WBCs, negative IgG index, no oligoclonal bands, negative viral PCR for HSV 1 and 2, VZV, CMV, and West Nile, and no malignant cells. EMG showed evidence of demyelination and frequent fasciculations with no evidence of denervation. Magnetic resonance imaging (MRI) of the brain and spine showed non-enhancing T2 FLAIR hyper intense signal changes in the ponto-medullary junction and the spinal cord extending from T10 to the conus medullaris. Initial diagnosis was NMO spectrum disease and the patient was started on IV pulse steroids for 5 days, followed by a course of oral prednisone of 60 mg daily. However anti Aquaporin-4 and anti-MOG antibodies were not detected in the serum. His symptoms worsened rapidly, and the weakness extended to both of his upper extremities. Repeat MRI of the brain and spine showed severe progression of the T2/FLAIR hyperintense lesions to the posterior pons, medulla oblongata and entire spinal cord. All parenchymal lesions were non-contrast enhancing. The cauda and conus medullaris had tumefactive appearance. Repeated CSF analysis showed elevated protein of 93, 5 WBCs, negative cultures, and negative viral PCR for CMV, VZV, HSV 1 and 2, but JCV PCR was positive. Follow up EMG showed progression of the disease with evidence of wide spread radiculopathy and anterior horn cell involvement. Prednisone was gradually tapered off. His condition continued to deteriorate with involvement of respiratory and bulbar muscles. Given the extension of the disease and poor prognosis, the family withdrew care after 1 month of hospital stay and declined autopsy. Conclusion: PML is a fatal disease that should be suspected in immunosuppressed patients with rapid neurological decline. Typically, it affects the brain and the cerebellum, however it should be included in the differential diagnosis for patients LETM, particularly if the lesions are non-contrast enhancing. JCV PCR is moderately sensitive but highly specific as a useful tool for diagnosis, however biopsy is remains gold standard for diagnosis. While no effective treatment has been identified reconstitution of the immune state might suppress the viral replication.
Presentation Date
5-2019
Recommended Citation
Mohamed, Ghada A.; el Din Osman, Gamal; Abd El Noor, Hassan; Newman, Daniel; and Katramados, Angelos, "JC Virus Induced Longitudinally Extensive Transverse Myelitis in Immunocompromised Patient" (2019). Case Reports. 56.
https://scholarlycommons.henryford.com/merf2019caserpt/56