Files
Download Full Text (365 KB)
Program
WSU Medical School
Training Level
Medical Student
Institution
Wayne State University
Abstract
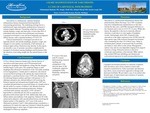
Background: Sarcoidosis is a multisystem, immune-mediated inflammatory disease characterized histologically by noncaseating granulomas. The underlying etiology favors a multifactorial origin with genetic predisposition, however it remains largely unknown. Presenting symptoms commonly include dyspnea, cough, and chest pain, as more than 90% of individuals with sarcoidosis have pulmonary involvement. Laryngeal involvement is rare and most frequently accompanies diffuse disease, with a reported incidence of 0.33-2.1%. Clinical manifestations of laryngeal sarcoidosis are typically chronic and include dysphagia, dyspnea, cough, and changes in voice quality; uncommonly, if left untreated, an inimical upper airway obstruction may develop. In this report, we describe a case of systemic sarcoidosis complicated by laryngeal involvement causing dysphagia and hoarseness with the intention of providing insight into the natural history of the disease. Case Report: A 55 yo African American female with a known history of sarcoidosis with lupus pernio and HTN presented with progressive dysphagia and dysphonia, noting that the changes initially began 2 years prior. Her symptoms began as mild dysphagia that advanced to limitations of her oral intake resulting in food regurgitation. 2 weeks prior to admission, she noticed occasional blood-spotting in the sputum she expectorated and developed a concurrent hoarse voice. CTPE was obtained in the ED showing bilateral axillary and hilar LAD. CT abdomen and pelvis also showed diffuse LAD involving the bilateral inguinal and retroperitoneal lymph nodes. ENT was consulted and performed an excisional biopsy of a lymph node in the left axilla for concern of diffuse LAD. Results from this biopsy demonstrated noncaseating granulomas, findings consistent with systemic sarcoidosis. A FFL showed a hypomobile to immobile left AE fold on inspiration and phonation with normal right AE fold. Additionally, there was diffuse edema and erythema of the epiglottis, bilateral AE folds, and posterior pharynx, with sarcoid-related lesions involving the lingual surface of the epiglottis. A CT scan of the neck is illustrated in figure 1. After pulmonology consultation, a prednisone 4-6 week slow taper was initiated to which the patient immediately began to show signs of improvement and was discharged to follow-up outpatient. Discussion: Sarcoidosis is a multisystem inflammatory disease that predominately affects the lungs. Up to 30% of patients may have extrapulmonary manifestations at sites that include the skin, eyes, and CNS; laryngeal infiltration is less frequent and is seen in 0.33-2.1% of cases. Within the larynx, the epiglottis is the most commonly affected structure, in part due to its rich supply of lymphatic vessels. Interestingly, about 54% of patients with sarcoidosis of the upper respiratory tract (SURT) have the lupus pernio type, with exclusive laryngeal involvement only constituting less than 1/3 of those cases. Delay in treatment places patients at increased risk for mortality secondary to mass effect on the airway. Management options vary and are case dependent ranging from surgical resection of large obstructive lesions to the more commonly used systemic corticosteroids. Other options may include CO2 laser debulking and intralesional corticosteroid injections for well-circumscribed lesions. Conclusion: Laryngeal involvement presents in a minority of patients with sarcoidosis and is more common in those with cutaneous manifestations. Early assessment and detection may allow a more conservative approach to therapy with decreased morbidity. We provided a case of our patient who showed signs of improvement upon initiation of systemic corticosteroid therapy.
Presentation Date
5-2019
Recommended Citation
Shukairy, Mohammad; Modi, Sunjay; Murad, Ahmad; and Gorgis, Sarah, "A Rare Manifestation of Sarcoidosis: A Case of Laryngeal Infiltration" (2019). MERF 2019 - Case Reports. 115.
https://scholarlycommons.henryford.com/merf2019caserpt/115