Files
Download Full Text (814 KB)
Program
Pathology
Training Level
Resident PGY 2
Institution
Henry Ford Hospital
Abstract
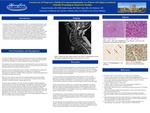
Progressive multifocal leukoencephalopathy (PML) is a rare demyelinating disease caused by reactivation of JC virus affecting typically subcortical and periventricular white matter of immunocompromised hosts (HIV infection, hematologic malignancies). We present an unusual case of PML predominantly affecting cervical spinal cord and brainstem in an immunocompetent host. A 65-year-old female presented with vertigo, hemiparesis and right sided weakness. MRI of the brain without contrast showed T2 signal abnormality involving the medulla extending into the upper cervical cord to C2-C3 level. Further work up showed positive ANA, elevated SS-A/Ro and SS-B/La antibodies consistent with Sjögren Syndrome. The patient deteriorated rapidly, expiring eight days after onset of acute respiratory failure. Autopsy showed multifocal white matter lesions with perivascular lymphocytic cuffing, microglial nodules, influx of activated microglial and numerous oligodendroglial nuclei with ground glass inclusions in the spinal cord, brain stem, cerebellum and cerebral hemisphere. The inclusions were immunoreactive with Simian virus-40 (SV-40), P53 and MIB-1 immunostains. The distributions of the lesions were predominantly in the medulla and upper cervical cord, correlating with pre-mortem MRI. A rare subset of PML cases can occur in association with connective tissue disorders (Sjögren in this case), Systemic Lupus Erythematosus (SLE) being the most common. Predominantly spinal involvement by PML is also rare. PML should be considered in the differential diagnosis of spinal cord/brainstem lesions, particularly in the patients with connective tissue disorders. This highlights the importance of post-mortem examination in selected cases without definite clinical diagnosis.
Presentation Date
5-2019
Recommended Citation
Onwubiko, Ifeoma; Taneja, Kanika; Gupta, Nilesh; and Mukherjee, Abir, "Progressive Multifocal Leukoencephalopathy Presenting as Transverse Myelitis" (2019). Case Reports. 65.
https://scholarlycommons.henryford.com/merf2019caserpt/65