Files
Download Full Text (550 KB)
Program
Ophthalmology
Training Level
Resident PGY 2
Institution
Henry Ford Hospital
Abstract
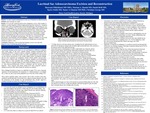
Background: Primary lacrimal sac tumors are a group of rare, highly malignant group of orbital neoplasms. Early diagnosis is critical, but often delayed, as these tumors are commonly mistaken for comparatively benign conditions. To our knowledge, there are less than 15 published cases of primary lacrimal sac adenocarcinoma. Purpose: To report a rare case of primary lacrimal sac adenocarcinoma with surgical removal and reconstruction by oculoplastics, orthopedic surgery and otolaryngology. Methods: Interventional Case Report. Results: A 55-year-old woman presented with six months of right periocular edema and tearing. Lacrimal gland irrigation revealed a nasolacrimal duct obstruction (NLDO). She underwent dacryocystorhinostomy (DCR) with Crawford stent placement for presumed chronic dacryocystis (lacrimal sac infection). Lacrimal sac pathology was unremarkable. One year later, she presented with recurrent symptoms. CT of the orbits showed a right nasolacrimal mass extending from the lacrimal fossa through an enlarged nasolacrimal duct. Nasal endoscopic biopsy with otolaryngology demonstrated poorly-differentiated glandular structures with AE1/AE3 and CK7 positivity, diagnostic for adenocarcinoma. PET-CT showed no other areas of hypermetabolic activity so she was determined to have Stage II (T2N0M0) poorly differentiated carcinoma. The patient was discussed at tumor board. Surgical intervention with adjuvant radiation therapy was recommended. Oculoplastics, otolaryngology and orthopedic surgery collaborated in a 13 hour lacrimal sac excision and orbital reconstruction. After dacryocystectomy and frozen sections, she was determined to have clear surgical margins (<1mm). The orbital floor, inferior rim and medial wall were repaired with a porous polyethylene coated titanium fan implant. The eye was spared and never incised. A harvested forearm graft of radial bone and forearm tissue reconstructed the right maxilla. Anastomoses of the radial artery to facial artery was performed. Tissues were closed with the aid of a rotational forehead flap. Over the last three months, radiation oncology has administered 60Gy of radiation. Fortunately, she has had no evidence of tumor recurrence or metastases. She continues to follow closely with oculoplastics, otolaryngology, orthopedic surgery and radiation oncology. Conclusion: Primary lacrimal sac tumors are exceedingly difficult to diagnose and treat, necessitating a multidisciplinary collaboration between medical specialties. Our case represents a treatment paradigm for eye sparing primary lacrimal sac adenocarcinoma excision and reconstruction. Continued medical provider education and improved treatment algorithms are essential to maximize patient outcomes.
Presentation Date
5-2019
Recommended Citation
Mikkilineni, Shravani; Brill, Daniel; Fields, Taylor; Hamid, Mariam; and George, Christian, "Nasolacrimal Duct Obstruction Caused by Primary Lacrimal Sac Adenocarcinoma" (2019). Case Reports. 71.
https://scholarlycommons.henryford.com/merf2019caserpt/71