Files
Download Full Text (839 KB)
Program
Internal Medicine
Training Level
Resident PGY 2
Institution
Henry Ford Hospital
Abstract
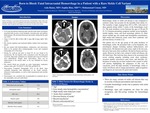
Case: The patient is a 25 YO African American male with S/Oarab sickle cell anemia who presented with an acute, severe headache, extremity pain, and hallucinations. He presented distressed and tearful, stating that his pain was 10/10. His initial vitals showed that he was afebrile (36.5F), normotensive (123/83), with a heart rate of 71 bpm, a respiratory rate of 18 bpm, and a saturation of 96% on room air. His physical exam was only remarkable for slowed cognition and emotional lability without focal neurologic deficit. He was treated with hydromorphone, ondansetron, and intravenous fluids as he awaited chest roentgenography (x-ray) and computed tomography (CT) of his head. Initial labs revealed a leukocytosis of 14.4 g/dL, a hemoglobin of 10.9 g/dL at the patient’s baseline, MCV 103.1, and platelet count of 445 g/dL. Basic metabolic panel revealed a normal creatinine and electrolytes. His coagulation panel showed a slightly increased PTT at 17 seconds and an INR of 1.43. No serum lactate dehydrogenase (LDH), liver function tests, or reticulocyte count were ordered. During his work-up and prior to head CT, he was found to be unconscious. He was hypoxic with a saturation in the 30s with good waveform. Bag-mask ventilation was initiated and 6 mg of IV Narcan were administered. Despite these interventions, there was no improvement in his mental status, so he was intubated for airway protection. His arterial blood gas revealed an acute hypercapnic respiratory acidosis with a pH 7.18, PCO2 71, PO2 260, and HCO3 25. He was sent emergently for head CT. It revealed a large cerebellar hematoma with obliteration of the fourth ventricle, obstructive hydrocephalus, as well as both transtentorial and tonsillar herniation. Neurosurgery was consulted who recommended no treatment due to the catastrophic, non-survivable bleed.
Discussion: Hemorrhagic stroke in sickle cell disease is rare compared to ischemic stroke, but accounts for the majority of the mortality from stroke in sickle cell disease [1, 2]. The peak incidence of hemorrhagic stroke occurs between the ages of 20 and 29 [2, 3]. Risk factors for hemorrhagic stroke in sickle cell include age, low steady-state hemoglobin concentration, and high steady-state leukocyte count [2]. There is a high mortality associated with hemorrhagic shock in sickle cell with 25% to 50% of these patients dying within 2 weeks of the hemorrhagic event [1]. Common presenting symptoms include severe headache, nuchal rigidity, coma, and focal neurologic deficit [1]. Our patient, in the age group with the peak incidence of hemorrhagic stroke in sickle cell, presented with a severe headache and a leukocytosis. He had previous pain crises, but never had acute chest syndrome. Although less studied, our patient had a rare variant of sickle cell anemia, the S/Oarab form. This form has been shown to be associated with severe sickling sequelae [4]. Incidence of stroke has not been studied in this variant of sickle cell anemia. In conclusion, sickle cell anemia is associated with increased rates of hemorrhagic stroke, often with patients presenting with severe headache and altered neurologic exam. Due to its high mortality, rapid recognition and diagnosis are necessary for quick intervention.
Presentation Date
5-2020
Recommended Citation
Ramo, Aula; Binz, Sophia; and Usman, Muhammad, "Born to Bleed: Fatal Intracranial Hemorrhage in a Patient with a Rare Sickle Cell Variant" (2020). Case Reports. 30.
https://scholarlycommons.henryford.com/merf2020caserpt/30