Files
Download Full Text (1.0 MB)
Program
WSU Medical School
Training Level
Medical Student
Institution
Wayne State University
Abstract
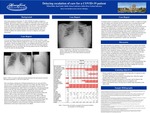
Background: Since being reported on December 31st 2019, COVID-19 has become a pandemic. In Detroit, there are 1075 cases and 23 deaths, as of March 28th, 2020. Rapid identification of the disease is vital as preliminary reports show that multiple ED and clinic visits are associated with worse outcomes, likely due to delayed treatment. Our report describes the course of a COVID-19 patient who required multiple visits prior to diagnosis, and rapidly deteriorated.Case Report: A 63-year old African American man presented to his PCP with sore throat, cough, and body aches. Patient endorsed symptoms for 4 days, no sick contacts, and flu swab was negative. Patient was diagnosed with a viral syndrome and prescribed rest and symptomatic care. The following day he went to the ED with worsening symptoms and hypotension and was sent home. The next day, patient went for a CXR, where he developed SOB. Due to his distress and presence of bilateral pneumonia, he was sent to the ED rule out COVID. At the ED, patient endorsed a fever, SOB, and chills. Patient’s past medical history included asthma, hypertension, and diabetes. On exam, he was febrile but hemodynamically stable. Patient was ill-appearing, with decreased breath sounds on the left. Labs showed leukopenia, lymphopenia, and an AKI. COVID testing was sent. Patient was admitted, with airborne plus precautions, and antibiotics were started.On hospital day 3, patient became persistently febrile and hypoxic. ABG was done which showed a PaO2 of 55.9. Due to worsening respiratory status, patient was intubated and transferred to the MICU. CXR was repeated and showed worsening airspace opacities bilaterally, and small pleural effusions. COVID test came back positive and treatment began with Hydroxychloroquine, and use of remdesivir pending. On hospitalization day 7, patient received remdesivir and tocilizumab, with hopes that reduced systemic inflammation would lead to improvement of his ARDS. Overnight, patient was hypotensive and nonresponsive to fluids. Levophed was begun, and vent settings were increased. On days 9 and 10, due to worsening hypoxia and inability to follow commands, patient was paralyzed to allow for more time to improve inflammation. Patient was placed on max vent settings, and his PaO2 sat was 57. CXR was repeated due to worsening vent requirements and showed no change. Subsequently, patient became tachycardic in the 120s, and hypotensive to the 80s. D-dimer was elevated, and patient desaturated when turned or repositioned. On day 11, patient was found to be hyperkalemic. Nephrology was consulted and determined the hyperkalemia was due to hemolysis secondary to DIC, but the patient was not a candidate for ultrafiltration or intermittent dialysis. Due to absence of clinical improvement, patient was transferred to comfort care, and expired.Discussion: Our report elucidates the importance of rapid identification of a patient with COVID. Our patient had a standard presentation with cough, fever, body aches and sore throat, indicating that the possibility of COVID as the cause for the patient’s presentation should have been considered. During a pandemic it is vital to practice with a high of index of suspicion. The importance of prompt identification of the illness becomes even more salient considering that current treatment approach is primarily symptomatic management, due to lack of clinically effective curative treatments. It may seem overly simplified, but the sooner a patient is able to receive these services, the more likely they are to recover. While our patient had multiple risk factors for deterioration due to COVID, such as HTN, and T2DM, our patient had two opportunities for escalation of care and identification of his underlying pathology that could have improved his prognosis. Further, our report is in line with preliminary findings that African Americans and patients
Presentation Date
5-2020
Recommended Citation
Rakic, Nikola; Fadel, Raef; Abreu-Lanfranco, Odaliz; Brar, Indira; and Suleyman, Geehan, "Delaying escalation of care for a COVID-19 patient" (2020). Case Reports. 31.
https://scholarlycommons.henryford.com/merf2020caserpt/31