Files
Download Full Text (336 KB)
Program
Nephrology
Training Level
Fellow
Institution
Henry Ford Hospital
Abstract
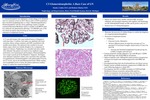
C3 Glomerulonephritis has undergone a recent change in its definition since its consensus review in 2013. Prior to 2013, C3GN would have been classified as a Type 3 Membranoproliferative Glomerulonephritis with the classic pathologic feature of double contoured Basement membrane which is notable in all MPGN types. It is relatively rare phenomenon affecting 1-2/1,000,000 cases in the US, based on registry data. A 71 year old woman with a past medical history of Hepatitis C with more than 1.5 million viral copies was admitted to the hospital with lower extremity edema, urinary retention, and CHF exacerbation with notable sacral edema. During her admission the patient began to have an acute kidney injury which was initially thought to be a component of aggressive diuresis. Nephrology was consulted and urine studies were obtained. The patient was noted to have nephrotic range proteinuria over 8 grams/gram and hematuria. Glomerulonephritis was a major concern given her Hepatitis C diagnosis. Serologies were obtained. Laboratory studies were consistent with a possible Cryoglobulinemic Glomerulonephritis with undetectable C4 levels, low C3 levels, and an elevated Rheumatoid Factor. While waiting for Cryoglobulin levels to return, the patient underwent a kidney biopsy to confirm the suspected diagnosis. Pathology results were inconsistent with Cryoglobulinemic Glomerulonephritis which were subsequently confirmed with undetectable Cryoglobulin levels. Instead the patient was diagnosed with C3 Glomerulonephritis. The biopsy was notable for a double contoured basement membrane, increased cellularity, mesangial expansion, and subendothelial humps. Given the biopsy results, the patient did not require pulse dose steroids, plasmapheresis or rituximab. Management was geared toward treating Hepatitis C to prevent the possibility of cryoglobulins forming in the future with plans to start immunosuppression with mycophenolate mofetil after. Although immunosuppression is the current standard of care for C3 glomerulopathy, data for all potential treatments of C3 Glomerulopathy to prevent progression to ESRD has been poor. Multiple cohort studies show about a 50% chance of ESRD within 10 years despite currently available treatments. This case illustrates the necessity of a kidney biopsy to confirm the diagnosis of a suspected glomerulonephritis. Although the patient had classic data suggestive of Cryoglobulinemic Glomerulonephritis, the results of the biopsy were consistent with an overactive complement system. This overdrive was not stimulated by unregulated cryoglobulins but instead by the Alternative Pathway. Obtaining a broad differential while not anchoring on a specific diagnosis prior to synthesizing all the data is vitally important in managing suspected glomerulonephritis.
Presentation Date
5-2020
Recommended Citation
Linder, Stanley and Shaban, Hesham, "C3 Glomerulonephritis: A Rare Case of GN" (2020). Case Reports. 57.
https://scholarlycommons.henryford.com/merf2020caserpt/57