Files
Download Full Text (409 KB)
Program
Podiatry
Training Level
Resident PGY 1
Institution
Henry Ford Wyandotte
Abstract
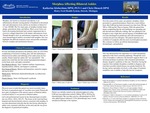
Clinical Presentation: 65-year-old female with past medical history of diabetes, hypothyroidism, and arthritis presented to the podiatry clinic on 12/21/2018 complaining of increased swelling, pain, and skin darkening to bilateral dorsal ankles and stiffening of her ankle joints for two months. Patient also had multiple hyperpigmented firm plaques on her back, neck, and all four extremities. Patient had recently been seen by her rheumatologist. Lab work from that visit revealed she was ANA+ and SSA+. The lesion on her neck was also biopsied and showed dermal sclerosis consistent with morphea (localized scleroderma). Therefore, she was diagnosed with morphea and Sjogren’s syndrome. It was then determined clinically that the skin lesions affecting her ankles were also consistent with morphea.
Treatment: Patient was initially started on CellCept in 2018 by her rheumatologist. She was then seen by a dermatologist in 2019 who added topical clobetasol, UVA1 phototherapy, and physical therapy to her regimen. In January 2020, the patient complained of worsening and spreading of the skin hardening and difficulty walking. She was admitted to the hospital to start a high-dose steroid regimen of SoluMedrol and was later discharged on prednisone. She continues to follow up with her rheumatologist, dermatologist, and podiatrist.
Conclusion: This case demonstrates the importance of a multi-disciplinary approach to this lower extremity pathology. Though the exact cause of morphea is unknown, the literature suggests there is an increased incidence in patients with concurrent autoimmune disease; Sjogren’s syndrome in this case. Therefore, having the expertise from multiple disciplines available to diagnose and treat these possibly related diseases was greatly beneficial. By having various specialties on board, a wide range of treatment modalities were available to alleviate her symptoms.
Presentation Date
5-2020
Recommended Citation
Kloberdanz, Katherine and Olenech, Chris, "Morphea Affecting Bilateral Ankles" (2020). Case Reports. 63.
https://scholarlycommons.henryford.com/merf2020caserpt/63