Files
Download Full Text (390 KB)
Program
Internal Medicine
Training Level
Resident PGY 1
Institution
Henry Ford Hospital
Abstract
Introduction: Statins are commonly prescribed in primary care offices daily; however, they are not exempt from adverse effects. Statin-induced myopathies are best described on a continuum, as patients can range widely in presentation. The most extreme of cases displaying respiratory distress, quadriparesis, dysphagia, and rhabdomyolysis. Cases on the severe end of the spectrum with respiratory failure are exceedingly rare and should be shared with the medical community in order to gain more insight into the types of statins most at risk for causing complications, most effective treatments based on disease severity, as well as characteristics and objective findings among affected patients in order to diagnose and treat in a time-effective manner.
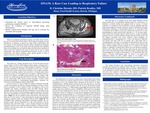
Case Description: The patient was a healthy, physically active 79-year-old male with past medical history of CVA in 2018 without residual deficits, controlled type 2 diabetes, HTN, and sleep apnea on CPAP presenting in February of 2020 with worsening quadriparesis, dysarthria, and dyspnea over the past 3 months. Physical exam revealed extreme muscle weakness of 3/5 in upper extremities, 4/5 in lower extremities, unable to raise arms above a 45 degree angle, normal cranial nerve exam. CT of the head/ neck was negative, moderate stenosis in carotid US of 50-60%, and MRI of head showing no acute changes. CPK elevated over 4,000 with elevated AST &ALT in the 300s. Autoimmune work up was nonrevealing. EMG showed possible myopathy vs motor axonal polyradiculoneuropathy vs demyelinating polyneuropathy. Treatment was conservative and discharged to subacute rehab (SAR). Over the course of 2 weeks at SAR, his weakness progressed with CPK >7,000 with continued elevated liver function prompting a transfer to Henry Ford for escalation of care in March of 2020. An exhaustive work up was completed with negative autoimmune panel and EMG showing chronic myopathy. History revealed he had been maintained on Atorvastatin 20 mg after his CVA in October of 2018 and began to manifest weakness in December 2019 with discontinuation in February 2020. MRI revealed diffuse muscular edema (Figure A). He was initially treated conservatively with intravenous fluids and over the course of 7 days had progressive dyspnea and dysphagia leading to respiratory failure and intubation. Muscle biopsy (Figure B) with anti-HMGCr IgG confirming statin-induced necrotizing myopathy. He was promptly treated with IV solumedrol for 5 days with transition to 60 mg prednisone daily with IVIG 2g/kg x 5 days. Despite treatment, the patient continued to decline with increasing CPK and inability to liberate from the ventilator. Given his prior wishes was terminally weaned per family request and passed soon after.
Discussion: The rapid decline of an otherwise healthy patient should prompt further inquiry as to the most efficacious treatment regimens; however, making the diagnosis can be challenging as it is a rare condition with a prevalence in less than 1% of statin-compliant patients. SINAM patients typically present with progressively worsening symmetrical proximal muscle weakness with CK levels in the thousands despite discontinuation of statins [1, 7]. Other findings include MRI showing muscle edema, atrophy, and/or fatty infiltration, positive anti-HMGCr, EMG positive for myopathy, and muscle biopsy displaying active necrosis [2]. Several case reports show widely varying time courses of 2 months to 10 years after the initiation of statin therapy to symptomatic necrotizing myopathies [2, 7]. Therefore, SINAM should be considered as a differential in the patient with new onset myopathies with past or current use of statins. The type of statins most likely to cause this condition were Atorvastatin, Simvastatin, Lovastatin, and Fluvastatin due to their lipophilic nature and ability to enter muscle cells [2]. Many patients are diagnosed when their most debilitating symptom is proximal muscle weakness; however, retrospective studies have shown that up to one-third of autoimmune myopathy cases had respiratory complications with 5 of these patients requiring intubation [4]. Our patient was unique in that despite the use of aggressive immunosuppression progressed to respiratory failure. To date there are no reported cases of death due to SINAM. This then begs us to consider, are all cases treated similarly? On the already murky topic of a standardized treatment regime for a rare disease, it is important to consider treating these patients based on severity of disease symptoms. It is standard of care for SINAM to stop the offending statin and begin immunosuppressive therapy. Treatment consists of prednisone with either methotrexate, azathioprine, or mycophenolate mofetil [1, 2], a third agent (IVIG or rituximab) can be added in severe cases; patients who received two or more immunosuppressive agents showed better outcomes [1, 2, 4]. In many studies, IVIG showed more favorable responses within the first 3 months of initiating treatment, however, its benefit seemed to dissipate after the 6 month mark [3, 4]. For patients presenting with severe weakness and/or dysphagia, IV methylprednisolone is recommended for 1-3 days with transition to high-dose oral steroids with taper, IVIG for 1-6 months, and a third agent such as cyclophosphamide, rituximab, or cyclosporine [3]. Rituximab has shown a great deal of benefit in many studies for its ability to increase muscle function and reduce immune-mediated muscular damage [3]. It is unknown the optimal dosage or combination of therapy that would be the most efficacious treatment, however, many studies have shown promise when using the agents described above. Due to the autoimmune nature of SINAM, relapses occurred often when immunosuppression is weaned or discontinued [1, 2, 4] and patients likely will require a life-long steroid-sparing agent [4]. There is no agreed upon maintenance therapy for these patients unable to be weaned off of immunosuppression and further studies are needed to answer this question.
Conclusion: Our patient presented with statin-induced necrotizing autoimmune myopathy that progressed to respiratory failure. SINAM is a rare complication of statin therapy that has high morbidity with rare mortality. SINAM should be on the differential in patients presenting with new onset progressive weakness who have been exposed to statin therapy. The mainstay of treatment is immunosuppressive therapy; however, the optimal regimen and duration is unknown and further studies are required to discern optimal treatment.
Presentation Date
5-2020
Recommended Citation
Hermiz, D. Christine and Bradley, Patrick, "SINAM: A Rare Case Leading to Respiratory Failure" (2020). Case Reports. 84.
https://scholarlycommons.henryford.com/merf2020caserpt/84