Files
Download Full Text (448 KB)
Program
WSU Medical School
Training Level
Medical Student
Institution
Wayne State University
Abstract
Background: Terson Syndrome refers to an intraocular hemorrhage in patients with severe subarachnoid hemorrhage (SAH), traumatic brain injury or intracerebal hemorrhage. The mechanism of injury is due to increased intracranial pressure which transmits into the optic nerve sheath and causes rupture of the retinal vessels. Despite its relatively common incidence, the syndrome remains under diagnosed or delayed because it usually occurs in severely ill patients with depressed level of consciousness. Early recognition of the intraocular hemorrhage on head CT and treatment can be significant to patient's outcome.
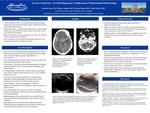
Case Description: We present a 46-year-old man with a past medical history of excessive EtOH use who presented to the emergency department with sudden onset of severe headache, nausea, and brief loss of consciousness. He acutely decompensated with tonic clonic seizure associated with hypertension, tachycardia, and vomiting. A stat head CT revealed subarachnoid hemorrhage involving the perimesencephalic cisterns, intraventricular hemorrhage, and hydrocephalus. CT Angiography revealed a left vertebral artery V4 dissecting-type aneurysm. Hunt and Hess Scale score was 2 and modified Fisher score was 4. An external ventricular drain (EVD) was inserted by Neurosurgery and he underwent cerebral angiography with deployment off low-diverting stent in the left vert V4 dissecting aneurysm. After extubation, the patient was complaining of bilateral blindness. Examination revealed inability to track movements, or blink to threat. It was believed that the vision loss was due to a bilateral posterior cerebral arteries (PCA) strokes versus manifestation of acute encephalopathy. Ophthalmology was consulted and fundus exam revealed bilateral vitreous and subhyaloid hemorrhages, concerning for Terson Syndrome. The patient underwent right eye pars plana vitrectomy for intraocular pressure relief. Retrospective review of head CT from admission showed bilateral crescentic hyperdensity in the posterior vitreous that is consistent with the diagnosis of Terson syndrome.
Conclusion: This case sheds light on the importance of early recognition of Terson Syndrome as a possible complication of sever SAH especially with high Hunt and Hess and Fischer scale scores as well as tell-tale signs of elevated intracranial pressure. In majority of cases, the syndrome remains undiagnosed in the early phase due to severity of patient’s illness and delayed clinical complaint of vision loss. This leads to delay in appropriate treatment and ultimately endangers patient's vision. In patients with severe subarachnoid hemorrhage, careful review of head CT for intraocular crescentic hyperdensity can prompt an early diagnosis of Terson Syndrome.
Presentation Date
5-2020
Recommended Citation
Gabe, Danielle; Alhajala, Hisham; Hamid, Mariam; and Howell, Bradley, "Terson’s Syndrome: An Underdiagnosed Complication of Subarachnoid Hemorrhage" (2020). Case Reports. 95.
https://scholarlycommons.henryford.com/merf2020caserpt/95