Files
Download Full Text (314 KB)
Department
Surgery; Surgery; Bariatric Surgery
Position/Job Title
Resident; Resident; General Surgeon
Description
Introduction: A rare complication following a sleeve gastrectomy is gastropleural fistula, which develops between the sleeve and the pleural space. This complication carries significant morbidity and mortality. This is a case report of a 73-year-old female presenting with a gastropleural fistula one year following a laparoscopic adjustable gastric band explant and conversion to a sleeve gastrectomy. She failed endoscopic management and required radical surgical intervention.
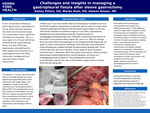
Case Description: The patient is a 73-year-old female with history of morbid obesity and a prior laparoscopic adjustable gastric band placement with weight regain. She underwent a laparoscopic band conversion to a sleeve gastrectomy in March 2022. Her postoperative course was relatively unremarkable. One year after her surgery, she presented with fever and shortness of breath. A chest CT scan revealed an 18 x 18 cm left empyema. She underwent a left thoracotomy and drainage in March 2023. A follow-up CT scan two months after her thoracotomy revealed recurrence of the left empyema, prompting an evaluation with an upper GI study, which revealed a gastropleural fistula to the left pleural space (Figure 1). She was referred for evaluation by bariatric surgery. In July 2023, a jejunostomy feeding tube was placed laparoscopically. Simultaneously, an esophagogastroduodenoscopy was completed, confirming the presence of the fistula in the proximal sleeve (Figure 2A), and a 23 x 100 mm covered stent was placed from the esophagus to the mid gastric body (Figure 2B). An upper GI study confirmed the resolution of the leak after stent placement. Enteral feeding was initiated through the jejunostomy feeding tube. Three months later, the stent was removed, and an upper GI study revealed a persistent leak. In November 2023, the patient underwent a robotic-assisted laparoscopic proximal gastrectomy, fistula takedown, and Roux-en-Y esophagojejunostomy (Figure 3). Her postoperative course was uncomplicated, and she was seen in the bariatric surgery clinic in January 2024 and was doing well.
Discussion: Gastropleural fistula following a sleeve gastrectomy usually has a delayed presentation. Timely diagnosis requires a high index of suspicion, which should prompt an investigation with a contrasted study to delineate the fistula. Nutritional support in the form of enteral nutrition through a jejunostomy feeding tube or total parental nutrition is essential for meeting caloric requirements and healing. Despite advances in endoscopic interventions including stenting, internal drainage, and endo-luminal VAC therapy, these techniques are often unsuccessful, and surgical intervention with gastric resection and Roux-en-esophagojejunostomy remains necessary.
Conclusion: Gastropleural fistula, a rare and morbid complication following a sleeve gastrectomy, presents a diagnostic and treatment challenge.
Publication Date
4-16-2024
Recommended Citation
Peters, Kelsey L.; Alam, Warda; and Nasser, Hassan, "Challenges and insights in managing a gastropleural fistula after sleeve gastrectomy" (2024). 2024 Henry Ford Jackson Hospital Research Symposium. 7.
https://scholarlycommons.henryford.com/hfjhrs2024/7